
Revenue growth is the second crucial aspect for healthcare providers after patient care, and it lies in flawless revenue cycle management healthcare. This financial operation aims toreduce claim denials and payment collection delays while evaluating faster reimbursement and increased cash flow.
Healthcare businesses that are more conscious about their financial performance stay with us. This guide explores an overview of the revenue cycle process in healthcare, management steps, benefits, and common challenges to avoid.
The healthcare revenue cycle management is defined as a revenue process starting from patient scheduling appointments and ends at collecting payment and reporting. This process cycle facilitates practitioners to collect each penny for the service they deliver to patients.
There are many major RCM roles, including insurance processing, registration, eligibility, coding, claims management, and revenue collection. Taking all these steps seriously leads to better revenue collection, satisfied patient experience, and, above all, helping your practices stay at the top of the healthcare business.
A well-targeted RCM system offers plenty of benefits for revenue cycle management. According to Global News, the RCM market is expected to grow to around USD 453.47 billion by 2034.
Revenue cycle operations improve communication by integrating EHR with accounting systems for better billing processes and faster reimbursement.
It offers flawless, accurate medical codes and claims for quicker reimbursement and lower financial stress.
RCM streamlines the error-free billing process, which fills the gap between patients getting service and practitioners getting paid.
The administrative team will now be freed and could be more focused on patient care as RCM systems are designed to handle all revenue cycle components.
Revenue cycle healthcare systems assist providers in complying with ever-changing billing regulations and payers’ guidelines. Ultimately, it is beneficial for accurate claim submission.
A well-implemented RCM system shortened the revenue collection cycle by quickly registering, scheduling, applying, managing, and processing payments.
Engage patients throughout the process about costs, billing procedures, and payment to improve their satisfaction so they keep coming back.
An efficient RCM assists providers by replacing the manual billing with an automated process that handles every step, such as claim submission, denial management payment collection, and compliance management. This not only reduces administrative burden but also decreases overhead costs by reducing billing errors and delays.
The healthcare revenue cycle system provides real-time access to all financial data, which means 100% transparency in the revenue cycle. It includes clear billing payments, detailed cost breakdowns, and easy-to-understand payment options to boost trust among patients and doctors.
The healthcare revenue cycle process is an entire financial process practices follow. It includes all clinical and administrative functions that contribute to revenue generation and reimbursements. The revenue cycle includes the below general steps:

Revenue cycle management in healthcare (RCM) involves active management and optimization steps that enhance the above revenue cycle process. Without wasting time, let’s elaborate on the important steps in revenue cycle management.
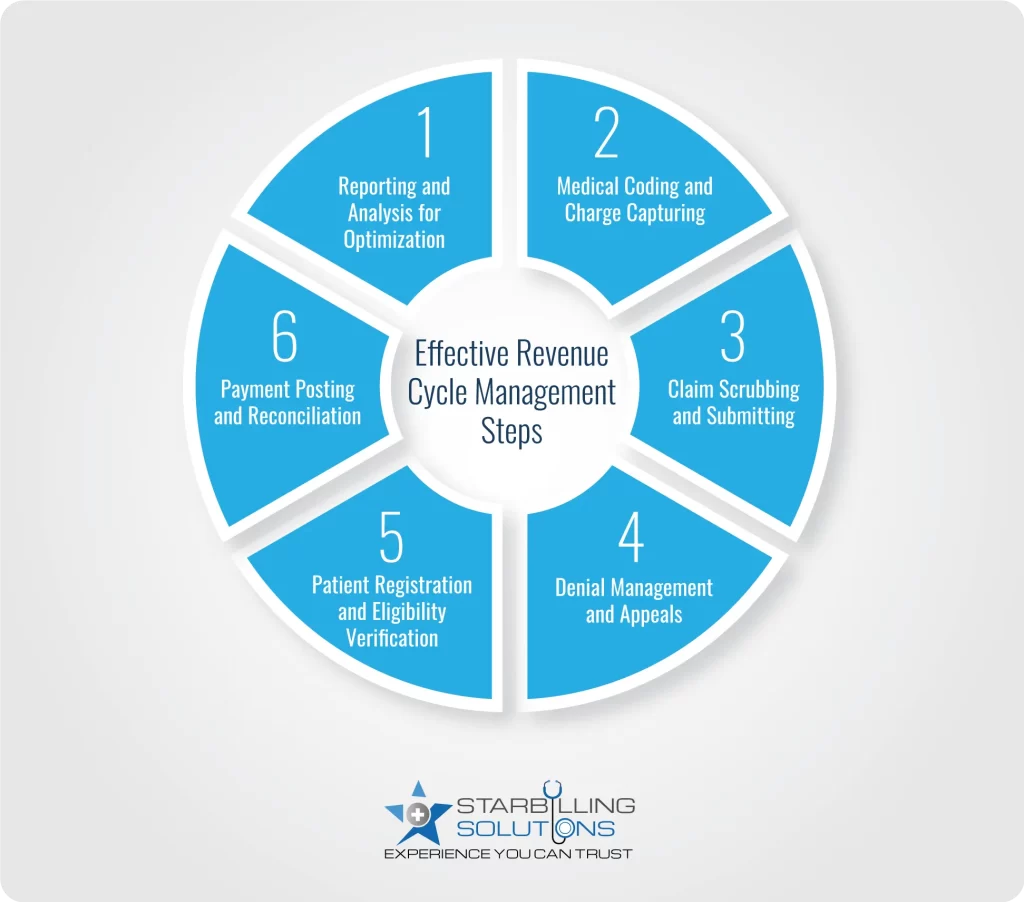
The revenue cycle management process in healthcare begins by registering the patient, either through front office staff or via a patient portal. This provides the practices with access to necessary patient information, which is later used to verify patient insurance.
These steps in revenue cycle management in healthcare are essential for providers for two purposes. Firstly, whether patient information is accurate and he/she is allowed to schedule a meeting. Secondly, if the patient has active insurance coverage, what are their terms? Also, how much does a patient have to pay out of pocket besides the insurance?
As soon as the patient receives medical services, convert them into appropriate codes. This healthcare revenue cycle management process step includes translating medical procedures, diagnoses, and services into ICD-10 and CPT-9 codes. Manual coders or automated coding tools integrated within healthcare IT platforms enter these medical codes.
The next step involves entering charges in the billing system based on medical codes and practitioners’ fee schedules. The charge entry needs to be accurate as it directly impacts the claim accuracy and total amount of reimbursement.
Once medical services are properly coded, they are sent for a claim scrubbing process. This involves reviewing medical claims for errors before submitting them to payers. The scrubbing process analyzes various issues, such as invalid codes, incorrect patient information, incomplete documentation, etc.
Nowadays, modern claims are submitted electronically through the EDI (Electronic data interchange) processing or ERA (Electronic remittance advice) platform to ensure accuracy and faster reimbursement. Payers validate that the claims comply with payment policies and agreements to decide whether they should be denied or paid fully or in half.
If the claim is denied, revenuecycleclaimsmanagement and appeals take place. This process means the claim does not follow payer guidelines, and they rejected it. Major reasons for denial could be missing patient information, coding errors, eligibility issues, etc.
At this stage, the denial management service finds denial errors and resubmits the appeal to payers for quick approval. Additionally, every reason for claim rejection is recorded to prevent repetitive future denials.
Payment posting and reconciliation are the next steps in revenue cycle management. The payment posting process is responsible for recording and reconciling receivable payments from payers and patients to healthcare providers for the services they offer.
The reconciliation process balances the record payments with the expected payment to ensure accurate recovery and avoid discrepancies. Perfectly completing these processes is essential for ensuring accurate payments are collected for the practice revenue cycle.
The last steps of revenue cycle management are actively analyzing and reporting key monitor indicators and industry trends. When providers use these insights, they are able to flag potential areas of improvement in overall RCM and implement innovative strategies to optimize financial performance.
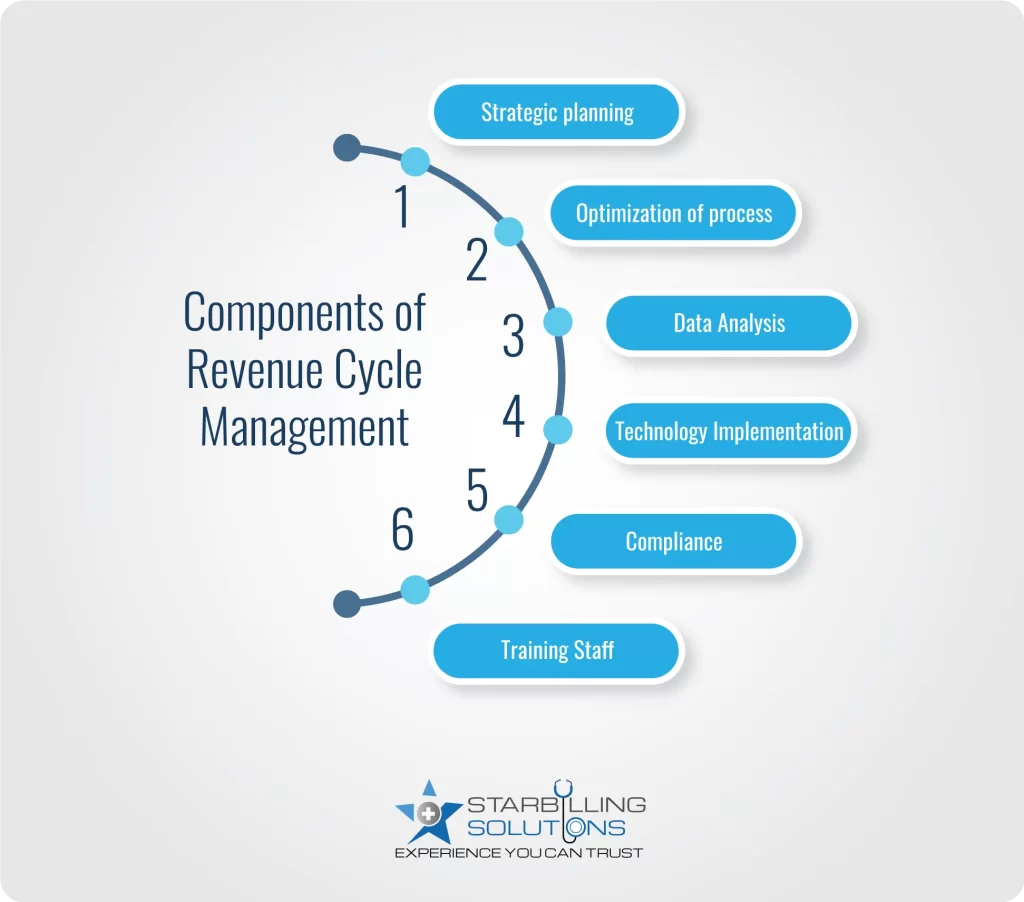
The key components of revenue cycle management are strategy making, process optimization, data analysis, compliance, and staff training. Each one is elaborated on below.
A recent study revealed that $262 billion in healthcare claims are initially denied, a big loss of revenue caused by major challenges in RCM. Get to know these challenges in revenue cycle management healthcare to maximize financial return.
Monitoring frequent updates and changes in billing and coding regulations is challenging for effective revenue cycle operations.
Healthcare providers relying on digital systems for effective medical billing revenue cycle could be more prone to vulnerable cybersecurity breaches, resulting in lost revenue and reputational damage to the organization.
Inability to track and analyze key medical revenue cycle management metrics, including net collection rate, denial rate, days in accounts receivables (AR), bad debt rate, and clean claim rate.
Lack of healthcare revenue cycle management staff training, insufficient knowledge, and higher turnover are significant challenges in revenue cycle management healthcare, leading to financial loss.
Insufficient authorization for patient and clinical data before claims submission leads to excessive claim denials, which affects the revenue cycle in healthcare.
RCM brings technology integration challenges such as technological overload, compatibility, and data security issues. This can slow down claim processing and cause mistakes that hurt revenue cycle performance.
As you expand your small healthcare organization, at some point in time, you may encounter rising technology costs for billing and frequently changing regulations. These could pose complexities for your in-house team in implementing effective revenue cycle management in healthcare.
That’s why, in the past decade, most practices have relied on outsourcing RCM services such as medical billing, coding, denial management, and AR follow-up to optimize financial growth. Third-party RCM services have access to industry experts and advanced-level tools and technologies for Flawless billing purposes. Hiring them assists practices in freeing their in-house RCM team and focusing more on patient care while letting experts handle their revenue.
A revenue cycle begins in healthcare when a patient schedules a meeting with a healthcare provider or seeks assistance related to any medical situation. The process ends when practices get paid for the services they offer to patients.
RCM stands for revenue cycle management in medical billing, which consists of a series of steps. Healthcare providers take these steps to ensure they receive payment for the services they provide.
The goal of revenue cycle management optimization is to provide actionable insights into current revenue cycle operations over time, with the aim of correcting problem areas, improving productivity, reducing costs, and increasing revenue.
The three primary pillars of revenue cycle healthcare are people, process, and technology.